Ovarian PRP application is a procedure in which a patient’s own blood components are processed and injected into the the ovarian cortex for the purpose of initiating/supporting the process of oogenesis. With recent developments in medical imaging as well as laboratory practices, existence of ovarian stem cells has come to light. These ovarian stem cells have been shown to have a potential for oogenesis, pregnancy and live birth. Initially, animal models provided evidence for such potential while later human models have shown resumption of menstrual cycles in menopausal women, improvement in ovarian function and oocyte growth and development. With ovarian PRP applications, there are a number of considerations that are important for a succesful outcome:
1- Platelet concentration: Platelet rich plasma is the part of our blood that has higher platelet content compared to the rest of our blood. With ovarian PRP applications, we concentrate the platelet numbers in your plasma and elevate the already high numbers up to 5 times it’s normal value. We measure your platelet count prior and post plasma processing in our labs and make the results available for our patients so they can see for themselves how much the platelet content has increased.
2- Inactivation/Activation protocols: Platelets can be spotaneously activated during the laboratory work. We need to time their activation so that they are activated inside the ovaries, not prior. Therefore, this step is one of the most vitals steps that determine the fate of platelets.
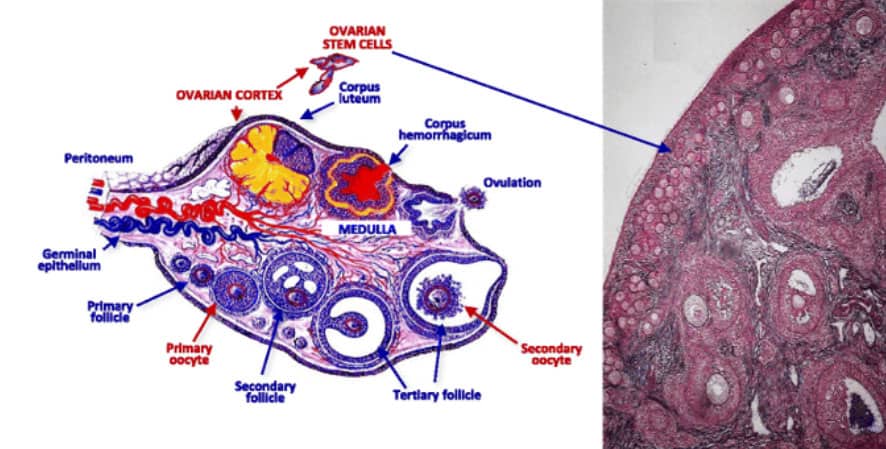
3- Site of injection: Ovarian stem cells are located in specific parts of the ovaries. Targeting these tissues is important for an effective treatment.
4- Post-PRP supplementation: Platelets contain growth factors, enzymes, co-factors and many other proteins. These are all involved in a number of physiological events, including cellular growth and proliferation. Given our aim is to initiate/support oogenesis (oocyte development and maturation), we need as much biological support as we can get. PRP is one key component to provide this support. However, there are other components that play a role in cellular development as well as genetic integrity of cellular processes. One of these is the growth hormone.
Human growth hormone is a naturally produced hormone in our bodies that support cellular growth and development. As we age, the production also slows down. Following ovarian PRP treatment, we aim to initiate production of oocytes and human growth hormone helps support growth the oogenesis process. For this, we will recommend a 10-week use of low dose human growth hormone supplementation. HGH has been shown in our own clinical experience to improve oocyte’s genetic integrity when administered in low dosages approximately for 10 weeks prior to oocyte collection. The efficacy and the use of growth hormone is well reported in IVF treatments. However, it is purely our own protocol to use human growth hormone alongside with ovarian PRP, which is essentially the same principle. Below is a link to some recent research on this:
https://www.frontiersin.org/articles/10.3389/fendo.2019.00502/full
https://www.ncbi.nlm.nih.gov/pubmed/29264990
Use of myoinositol supplementation has also been shown to imrpove oocyte quality in poor responders. Myoinositol has been shown to improve oocyte count and quality when used for at least 6 weeks prior to IVF treatment. In this context, we use it as an adjunct therapy to support the process of oogenesis for about 3 months prior to egg collection procedure (From the time of ovarian PRP until the time we collect the eggs during the IVF cycle). Below are some studies published showing the effects of inofolic supplementation prior to an IVF cycle:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4464995/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5350329/
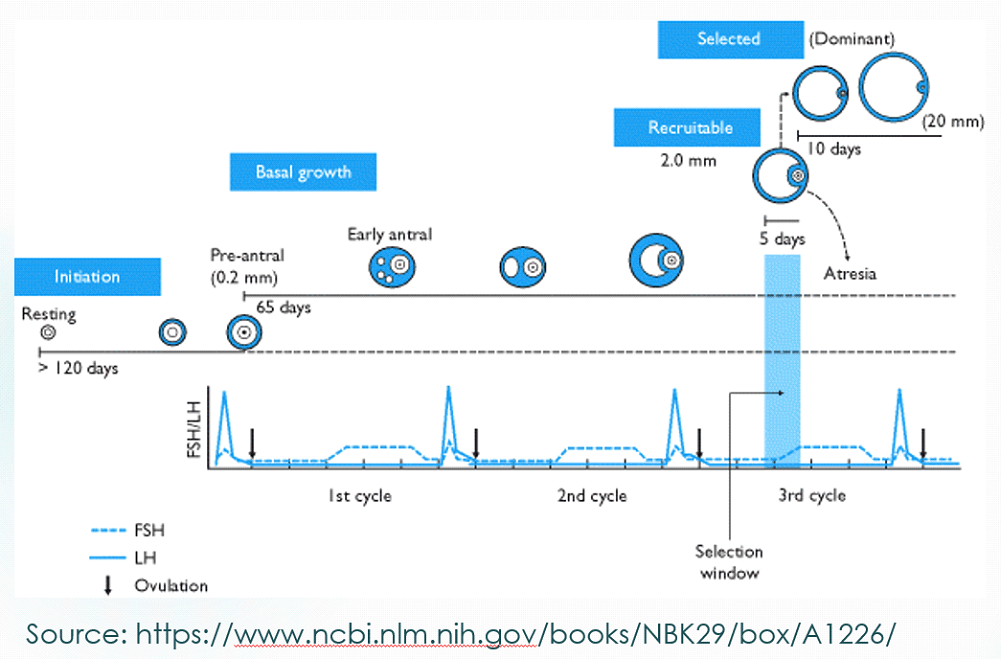
Patients in younger age brackets tend to benefit even more from ovarian PRP application as they still have a large pool of primordial follicles. Even when there is a problem with ovulation, it is often possible to stimulate primordial follicles into pre-antral and antral follicle line and initiate ovulation. This makes the primordial follicles our main target when treating patients in younger age brackets. We see better and quicker results in patients who are under the age of 40 who have premature ovarian failure.
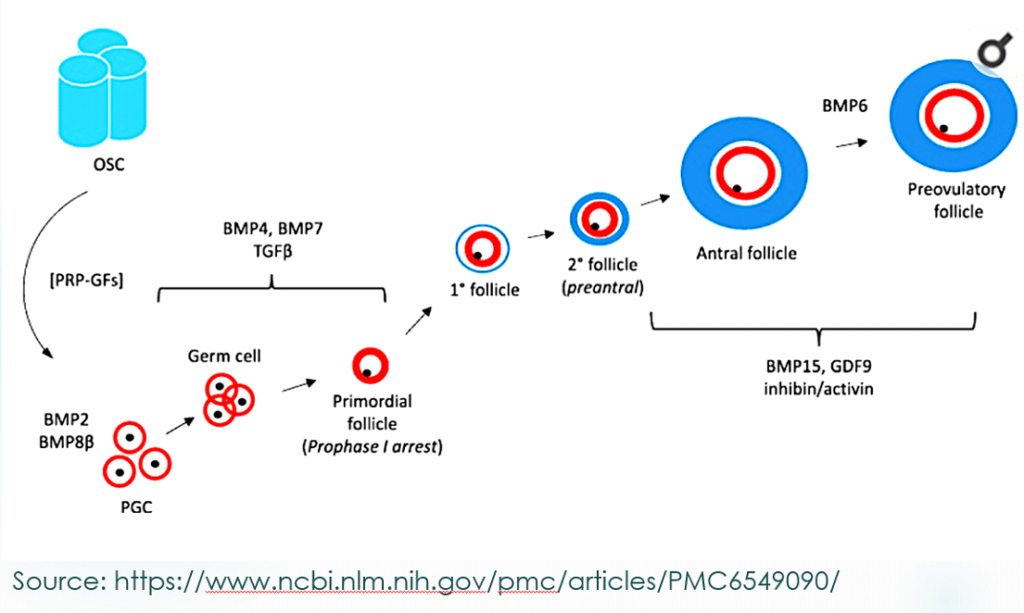
OSCs (ovarian stem cells) require growth factors in order to differentiate into the germ cell line. Once differentiation occurs, they follow the path of oogenesis. Similarly, primordial follicles, which are already differentiated from the germ cell line, are recruited directly into pre-antral and antral follicles.
Following ovarian PRP treatment, we have observed spontaneous resumption of menstrual cycles after menopause, spontaneous pregnancies with natural conception as well as IVF pregnancies. Given that we are not yet sure how long the full effects are likely to last, we try to plan treatment in a very strict timeline to exercise full effects from our treatments. For this purpose, immediately following a PRP application, we provide our patients with a calendar for taking supplements and for a subsequent IVF cycle. We require two sets of hormone testing. One set before PRP treatment, and one set two and a half months after PRP treatment. We usually ask that these tests are performed at the same laboratory for consistency of results. The purpose of these test results is to compare before and after results so that we can see for ourselves how successful the procedure has been. Based on the test results, we move forward with IVF treatment planning. The length of time between PRP application to egg retrieval in an IVF cycle is between 75 to 120 days, depending on age, pre-PRP profile and post-PRP testing.
We are one of the very first clinics in the world to start this application and we very well know that ovarian PRP application is not a mere injection of PRP into the ovaries. A well-designed treatment is necessary in order to appreciate the full effects of this ground-breaking scientific method.





Hi doctor
How much the cost of prp .
The cost of ovarian PRP treatment is 1,600 Euros, which covers the tests performed prior to your treatment.