- About
- Blog
- Infertility
- IVF Treatments
- New IVF Advances
- IVF Treatment in Cyprus
- IVF For Women Over 40
- IVF For Women Over 50
- IUI
- Mini IVF
- IVF + ICSI
- Cytoplasmic IVF
- Tandem IVF Cycle
- Egg Donation
- Embryo Donation
- Sperm Donation
- Gender – Sex Selection
- Gestational Surrogacy
- Same Sex Gay Surrogacy
- Surgical Sperm Retrieval
- Pre Implantation Genetic Diagnosis PGD
- Egg Freezing
- Gender Selection Using Donor Eggs
- Sickle Cell Disease Prevention
- F.A.Q.
- Travel
- About
- Blog
- Infertility
- IVF Treatments
- New IVF Advances
- IVF Treatment in Cyprus
- IVF For Women Over 40
- IVF For Women Over 50
- IUI
- Mini IVF
- IVF + ICSI
- Cytoplasmic IVF
- Tandem IVF Cycle
- Egg Donation
- Embryo Donation
- Sperm Donation
- Gender – Sex Selection
- Gestational Surrogacy
- Same Sex Gay Surrogacy
- Surgical Sperm Retrieval
- Pre Implantation Genetic Diagnosis PGD
- Egg Freezing
- Gender Selection Using Donor Eggs
- Sickle Cell Disease Prevention
- F.A.Q.
- Travel
Surgical Sperm Retrieval
Overview of Surgical Sperm Retrieval
Azoospermia is one of the main factors of infertility. It has been estimated that around 15% of all male infertility cases are due to azoospermia, which refers to complete absence of live sperm cells in the ejaculate. Causes of azoospermia are categorized into two groups. Obstructive azoospermia suggests that there is a blockage somewhere along the sperm delivery system and live sperm cells are not able to make it into the ejaculate as they are being blocked. Obstructive azoospermia could stem from a problem in one of the ducts that allow sperm to pass through. Infections are a common cause of this type of azoospermia. Non-obstructive azoospermia suggests that rather than a blockage, there is a problem with production of sperm and the testes are unable to produce any sperm at all. This can be due to testicular failures due to chromosomal abnormalities, varicocele which are known as benign cysts and hormonal problems. In any case, if you have had a semen analysis done, and the results indicate azoospermia, further investigation is to be carried out by a urologist for a complete diagnosis.
Before proceeding with treatment, it is very important that the male patient has been evaluated by his urologist and the precise reason for azoospermia has been established, whether obstructive or non-obstructive. Similarly, a post-ejaculate urinalysis is an important test to administer azoospermic men so that retrograde ejaculation can be ruled out as a possible explanation for azoospermia. If you are diagnosed with retrograde ejaculation, very simple methods of sperm isolation from your urine can be applied and the isolated sperm cells can be used for IVF treatment. A physical examination will also be indicative of possible causes of azoospermia. For instance, men with normal testes volume with bilaterally indurated epididymis or absent vas deferens can be identified as being azoospermic of obstructive etiology. On the other hand, presence of low testes volume and a history of cryptorchidism will indicate a case of azoospermia with non-obstructive etiology.
With recent innovations in medical technologies, surgical sperm extraction methods have become available. With any sperm retrieval procedure, there are three main goals to prioritize:
-To obtain the best quality of sperm possible with the surgical procedure. Given that the sperm sample which will be obtained will not contain mature spermatozoa found in normal sperm ejaculate, the surgeon still needs to do his best to retrieve the sperm cells that may be as close to the mature spermatozoa as possible, if the patient has viable sperm cells.
-To obtain a sufficient amount of sperm for fresh use during the IVF cycle and possibly for cryopreservation for a future cycle. Even though this is a very minor procedure, it is still a surgical procedure, so if possible, the procedure should aim to retrieve enough sperm for a few IVF cycles.
-To make sure that there is minimal damage to the reproductive tract when obtaining the sperm sample surgically so that future attempts at surgical sperm retrevial/extraction are not jeopardized.
Surgical sperm collection methods include the following:
1- Percutaneous Epididymal Sperm Aspiration (PESA)
PESA is a simple method of sperm extraction used for men who have an obstruction of the vas deferens, either due to vasectomy or other obstruction. In order to minimize scarring, PESA is usually done on one side. Although the sperm obtained with this procedure will be immature and lower quality sperm, majority of the time, PESA will yield enough sperm cells for the ICSI procedure. You should also keep in mind that the longer the time period you have been exposed to the obstruction, the lower the quality and quantity of sperm that can be obtained with this method. Therefore, younger patients often respond better to this method compared to men in more advanced age brackets. Similarly, although PESA yields good results for patients with vasectomy, the duration after vasectomy can be decisive whether a good sample is likely to be obtained.
2- Micro Epididymal Sperm Aspiration (MESA)
MESA sperm retrieval technique involves aspiration of sperm from the epididymis with a fine needle, which is a more advanced version of the PESA procedure. It is a surgical procedure and is carried out under a general anesthetic. Sperm extracted using this technique are often of poor quality but are usually suitable for freezing. In some cases, enough sperm might be collected for a number of ICSI procedures, allowing the patients to use part of the sperm for the ongoing fresh cycle and preserve some of it for a future cycle.
3- Testicular Sperm Extraction (TESE)
This method of sperm extraction is often used for non-obstructive type of azoospermia where sperm cannot be obtained from the epididymis. TESE procedure requires taking a small piece of tissue from the testis and isolating the sperm from this tissue. Compared to MESA or PESA, a lower number of sperm cells are likely to be extracted, and in some cases, viable sperm may not be found in the biopsy tissue, which may require canceling the cycle or opting for sperm donation.
It should be known that sperm samples extracted/retrieved via surgical methods will not be as mature as spermatozoa found in the ejaculate, therefore, success rates with surgically obtained sperm samples are likely to be lower compared to standard sperm samples. Furthermore, while in some cases it may appear that freezing the surgically obtained sample may be an option, viability of this sample is likely to be further reduced with the freeze/thaw procedures. It is always a good idea to use surgically retrieved sperm cells when they are fresh.
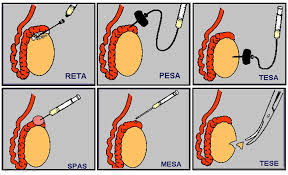
The diagram below shows how each of the surgical sperm retrieval methods are administered:
You may also be interested in our “Stem Cell Therapeutical Study” for Non-Obstructive Azoospermia.
North Cyprus IVF Centre
North Cyprus IVF Centre is a patient focused fertility clinic, located within “Elite Research and Surgical Hospital” in Nicosia, Cyprus. Our clinic is one of the most advanced fertility clinics in the world, offering a wider selection of treatment options at affordable prices.
Contact Us
Phone
English: +90 548 875 8000
French: +90 548 876 8000
Turkish: +90 542 869 8000
Arabic: +90 548 875 8000
German: +90 548 830 1987
Russian: +90 548 828 9955
info@northcyprusivf.net
© 2020 LowCostIVF - All rights reserved. Privacy Policy