- About
- Blog
- Infertility
- IVF Treatments
- New IVF Advances
- Mitochondrial Replacement Therapy!
- IVF Treatment in Cyprus
- IUI
- Mini IVF
- IVF + ICSI
- Cytoplasmic IVF
- Tandem IVF Cycle
- Egg Donation
- Embryo Donation
- Sperm Donation
- Gender – Sex Selection
- Gestational Surrogacy
- Same Sex Gay Surrogacy
- Surgical Sperm Retrieval
- Pre Implantation Genetic Diagnosis PGD
- Egg Freezing
- Gender Selection Using Donor Eggs
- Sickle Cell Disease Prevention
- F.A.Q.
- Travel
- About
- Blog
- Infertility
- IVF Treatments
- New IVF Advances
- Mitochondrial Replacement Therapy!
- IVF Treatment in Cyprus
- IUI
- Mini IVF
- IVF + ICSI
- Cytoplasmic IVF
- Tandem IVF Cycle
- Egg Donation
- Embryo Donation
- Sperm Donation
- Gender – Sex Selection
- Gestational Surrogacy
- Same Sex Gay Surrogacy
- Surgical Sperm Retrieval
- Pre Implantation Genetic Diagnosis PGD
- Egg Freezing
- Gender Selection Using Donor Eggs
- Sickle Cell Disease Prevention
- F.A.Q.
- Travel
IVF For Women Over 40
IVF treatment for Women over 40 at North Cyprus IVF
It is no secret that men and women both experience a decline in their level of fertility as they age.
However, this decline is more pronounced in women compared to men.
This is because men have active sperm production within their reproductive system throughout their lives while women are born with a finite set of ovarian reserves, which decrease with every menstrual cycle.
This difference in fertility allows men to biologically father a child even in more advanced age brackets while it becomes very difficult for women to conceive naturally after the age of 40.
The diagram below helps visualize the average rate of decline in ovarian reserves of an average woman throughout her lifetime.
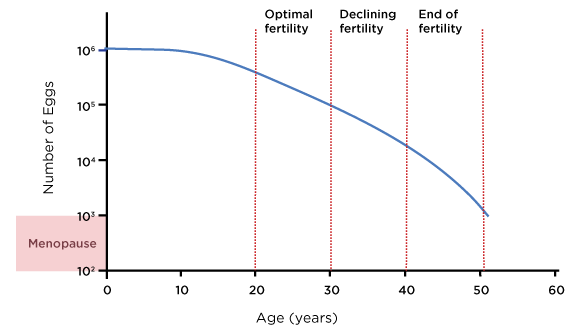
While the decline of ovarian reserves begins after menarche (first menstrual period after entering puberty), the rate of decline becomes very sharp after the age of 40. This means that both the count and quality of oocytes drop dramatically after the age of 40, making it very difficult for women over 40 to achieve a successful pregnancy using their own oocytes. After reaching menopause, there is still a minimal number of eggs is the reserves, but these eggs do not have the potential to ovulate or generate pregnancy.
One of the key factors when considering treatment options for women over 40 is an effective assessment of ovarian function. While some women may still have a very high level of ovarian function into their early 40s, some women will have very minimal to undetectable activity in their ovaries in the very same age bracket. Therefore, a careful assessment in necessary to identify the existing ovarian function in order to identify the right approach to a customized treatment protocol which will maximize chances of success. With every person comes a unique history. It is of utmost importance that we have a detailed history of your medical background so that we can better understand your situation and better help you. Based on ovarian function, previous reproductive history and previous fertility treatments, different approaches can be used for different groups of women. In this section, we talk about possible fertility treatment options at North Cyprus IVF Center for different groups of women based on their ovarian function.
Women over 40 with Normal to Optimal Ovarian Function (More than 10 Antral Follicle Count in total)
Women in their 40s, who are not able to conceive naturally, and who still have normal to optimal level of ovarian function can undergo treatment using their own eggs. However, it should be kept in mind that women in their 40s are more likely to have implantation failures and miscarriages due to oocyte (egg) aging. Aging of the oocyte does not only reduce their viability, it also affects the genetic integrity of the oocytes. This exposes the eggs to higher risk of genetic defects causing both implantation failures and early term miscarriages. It has also been shown that women over 40 are more likely to have a genetically abnormal child when they have a successful pregnancy to term. All of this means that there are risks associated with mothering a biological child after the age of 40.
While we take additional precautionary measures to help assist with embryo implantation, it makes sense to consider pre-implantation genetic screening as a method of embryo selection. Pre-implantation genetic screening through Next Generation Sequencing can help eliminate chromosomal aneuploidy, translocations as well as mosaicism. By selecting embryo(s) which are free of these genetic disorders, we can minimize the risk of genetic abnormalities in your child.
Women with normal ovarian function (more than 10 antral follicles in total between the two ovaries) who have undergone a number of IVF failures using own eggs
This group of women is different from the previous group in the sense that they have already undergone a number of IVF cycles with their own eggs and despite having a normal level of ovarian function, they have experienced negative cycle outcomes due to fertilization or embryo implantation problems. If uterine conditions are favorable and there are no other evident problems, oocyte quality becomes the main suspect. When a woman has an acceptable level of response to controlled ovarian hyperstimulation (more than 3 M2 quality oocytes), but these oocytes fail to fertilize or fail to implant despite a successful fertilization, alternative approaches can be considered. These can be:
1- Human growth hormone protocol aimed at improving genetic integrity of the oocytes. For more information on our human growth hormone protocols, please see our blog article on human growth hormone trials during IVF treatment.
2- If oocyte aging is the key consideration, Cytoplasmic Embryo Transfer can help improve the cellular energy levels of the eggs, thus allowing them to maintain normal function and become more viable for fertilization.
These two options can also be combined in order to assist the oocyte from both angles, increasing the likelihood of successful fertilization and therefore implantation and pregnancy.
Women with low ovarian reserves (Between 4 to 10 antral follicles in total between the two ovaries)
When ovarian function has declined and the level of reserves in the ovaries has dropped down to low levels of fertility, IVF success with using own eggs becomes less likely. This group of women are usuallt referred to as “poor responders”. While different IVF treatment protocols can be attempted and alternative medication brands and dosages can be utilized with the hopes of maximizing ovarian response, there is a limit to what medication protocols can achieve. Realistically speaking, even the most carefully designed treatment protocols will not generate a desired outcome simply because the ovarian reserves are insufficient. In such cases, the aim should be to maximize both the quality and the quantity of oocytes to be obtained. The quality aspect can be dealt with using measures recommended for the above groups of women. However, attempting an IVF cycle over the age of 40 with a result of 1 or 2 eggs is not a scenario that promises success. If you have had a similar experience with your previous IVF cycles where your egg retrieval procedure yielded 1 or 2 M2 quality eggs, which was not enough for an optimal number and quality of embryos for a successful embryo transfer, then embryo batching can be an option.
Embryo batching is a special sequential IVF treatment program where we perform a number of egg retrievals 3 months apart, create embryos either using standard ICSI protocols or more ideally, using cytoplasmic IVF treatment, and once we have a desired number of embryos, they can all be incubated to day 5 blastocyst stage, genetically screened for genetic abnormalities and then healthy embryos can be identified for an embryo transfer, maximizing the chances of success given the constraints imposed by declined levels of ovarian reserves.
Women with highly depleted ovarian reserves (less than 3 antral follicles and AMH levels of lower than 0.1 ng/mL)
If ovarian reserves are highly depleted and this is also evidenced by a low level of AMH and a low number of antral follicles, then prospects of obtaining viable eggs for a successful IVF cycle would be very unlikely. While we can do our best and design a treatment protocol to optimize your response, it is highly unlikely to obtain oocytes of fertilizable quality. In these cases, our recommendation would be to opt for IVF treatment using donor eggs. Using donor eggs can offer a chance of success up to 80%. If you are not yet ready to consider using donor eggs, then embryo batching can be an option as long as there is at least one embryo which can potentially reach cleavage stage (total of 8 cells on day 3 of development). It may take several attempts to obtain enough embryos to culture to the blastocyst stage and to perform genetic screening.
With recent technological advancements in the field of infertility, our IVF specialists now offer “ovarian rejuvenation” via platelet rich plasma injection into the ovaries. While this is still a brand new technology and there is only very limited information on its success, it is relatively free of any side effects and the cost of treatment is minimal. Therefore, if you are a woman over 40 with highly reduced ovarian function and you are not yet ready to give up on your eggs, our ovarian rejuvenation program may be for you.
Please contact us for more information.
North Cyprus IVF Centre
North Cyprus IVF Centre is a patient focused fertility clinic, located within “Elite Research and Surgical Hospital” in Nicosia, Cyprus. Our clinic is one of the most advanced fertility clinics in the world, offering a wider selection of treatment options at affordable prices.
Contact Us
Phone
English: +90 548 875 8000
French: +90 548 876 8000
Turkish: +90 542 869 8000
Arabic: +90 548 875 8000
German: +90 548 830 1987
Russian: +90 548 828 9955
info@northcyprusivf.net
© 2020 LowCostIVF - All rights reserved. Privacy Policy


